Pathophysiology[edit]
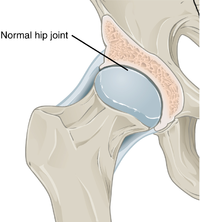
While OA is a degenerative joint disease that may cause gross cartilage loss and morphological damage to other joint tissues, more subtle biochemical changes occur in the earliest stages of OA progression. The water content of healthy cartilage is finely balanced by compressive force driving water out & swelling pressure drawing water in.[25] Collagen fibres exert the compressive force, whereas the Gibbs–Donnan effect & cartilage proteoglycans create osmotic pressure which tends to draw water in.[25]
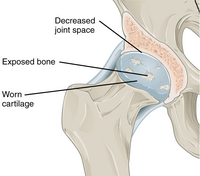
However, during onset of OA, the collagen matrix becomes more disorganized and there is a decrease in proteoglycan content within cartilage. The breakdown of collagen fibers results in a net increase in water content.[26][27][28][29][30] This increase occurs because whilst there is an overall loss of proteoglycans (and thus a decreased osmotic pull),[27][31] it is outweighed by a loss of collagen.[25][31] Without the protective effects of the proteoglycans, the collagen fibers of the cartilage can become susceptible to degradation and thus exacerbate the degeneration. Inflammation of the synovium (joint cavity lining) and the surrounding joint capsule can also occur, though often mild (compared to what occurs in rheumatoid arthritis). This can happen as breakdown products from the cartilage are released into the synovial space, and the cells lining the joint attempt to remove them.
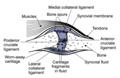
Other structures within the joint can also be affected.[32] The ligaments within the joint become thickened and fibrotic and the menisci can become damaged and wear away.[33] Menisci can be completely absent by the time a person undergoes a joint replacement. New bone outgrowths, called "spurs" or osteophytes, can form on the margins of the joints, possibly in an attempt to improve the congruence of thearticular cartilage surfaces in the absence of the menisci. The subchondral bone volume increases and becomes less mineralized (hypomineralization).[34] All these changes can cause problems functioning. The pain in an osteoarthritic joint has been related to thickenedsynovium[35] and subchondral bone lesions.[36]
Diagnosis[edit]
Diagnosis is made with reasonable certainty based on history and clinical examination.[37][38] X-rays may confirm the diagnosis. The typical changes seen on X-ray include: joint space narrowing, subchondral sclerosis (increased bone formation around the joint), subchondral cystformation, and osteophytes.[39] Plain films may not correlate with the findings on physical examination or with the degree of pain.[40] Usually other imaging techniques are not necessary to clinically diagnose OA.
In 1990, the American College of Rheumatology, using data from a multi-center study, developed a set of criteria for the diagnosis of hand OA based on hard tissue enlargement and swelling of certain joints.[41] These criteria were found to be 92% sensitive and 98% specific for hand OA versus other entities such as rheumatoid arthritis andspondyloarthropathies.[42]
Related pathologies whose names may be confused with OA include pseudo-arthrosis. This is derived from the Greek words pseudo, meaning "false", and arthrosis, meaning "joint." Radiographic diagnosis results in diagnosis of a fracture within a joint, which is not to be confused with OA which is a degenerative pathology affecting a high incidence of distal phalangeal joints of female patients. A polished ivory-like appearance may also develop on the bones of the affected joints, reflecting a change called eburnation.[43]






No comments:
Post a Comment