There are many possible pathophysiological mechanisms involved in the development and maintenance of obesity.[132] This field of research had been almost unapproached until the leptin gene was discovered in 1994 by J. M. Friedman's laboratory.[133] These investigators postulated that leptin was a satiety factor. In the ob/ob mouse, mutations in the leptingene resulted in the obese phenotype opening the possibility of leptin therapy for human obesity. However, soon thereafterJ. F. Caro's laboratory could not detect any mutations in the leptin gene in humans with obesity. On the contrary Leptinexpression was increased proposing the possibility of Leptin-resistance in human obesity.[134] Since this discovery, many other hormonal mechanisms have been elucidated that participate in the regulation of appetite and food intake, storage patterns of adipose tissue, and development of insulin resistance. Since leptin's discovery, ghrelin, insulin, orexin, PYY 3-36,cholecystokinin, adiponectin, as well as many other mediators have been studied. The adipokines are mediators produced by adipose tissue; their action is thought to modify many obesity-related diseases.
Leptin and ghrelin are considered to be complementary in their influence on appetite, with ghrelin produced by the stomach modulating short-term appetitive control (i.e. to eat when the stomach is empty and to stop when the stomach is stretched). Leptin is produced by adipose tissue to signal fat storage reserves in the body, and mediates long-term appetitive controls (i.e. to eat more when fat storages are low and less when fat storages are high). Although administration of leptin may be effective in a small subset of obese individuals who are leptin deficient, most obese individuals are thought to be leptin resistant and have been found to have high levels of leptin.[135] This resistance is thought to explain in part why administration of leptin has not been shown to be effective in suppressing appetite in most obese people.[132]
While leptin and ghrelin are produced peripherally, they control appetite through their actions on the central nervous system. In particular, they and other appetite-related hormones act on the hypothalamus, a region of the brain central to the regulation of food intake and energy expenditure. There are several circuits within the hypothalamus that contribute to its role in integrating appetite, the melanocortin pathway being the most well understood.[132] The circuit begins with an area of the hypothalamus, the arcuate nucleus, that has outputs to the lateral hypothalamus (LH) and ventromedial hypothalamus(VMH), the brain's feeding and satiety centers, respectively.[136]
The arcuate nucleus contains two distinct groups of neurons.[132] The first group coexpresses neuropeptide Y (NPY) andagouti-related peptide (AgRP) and has stimulatory inputs to the LH and inhibitory inputs to the VMH. The second group coexpresses pro-opiomelanocortin (POMC) and cocaine- and amphetamine-regulated transcript (CART) and has stimulatory inputs to the VMH and inhibitory inputs to the LH. Consequently, NPY/AgRP neurons stimulate feeding and inhibit satiety, while POMC/CART neurons stimulate satiety and inhibit feeding. Both groups of arcuate nucleus neurons are regulated in part by leptin. Leptin inhibits the NPY/AgRP group while stimulating the POMC/CART group. Thus a deficiency in leptin signaling, either via leptin deficiency or leptin resistance, leads to overfeeding and may account for some genetic and acquired forms of obesity.[132]
Public health
The World Health Organization (WHO) predicts that overweight and obesity may soon replace more traditional public health concerns such as undernutrition and infectious diseases as the most significant cause of poor health.[137][page needed] Obesity is a public health and policy problem because of its prevalence, costs, and health effects.[138] TheUnited States Preventive Services Task Force recommends screening for all adults followed by behavioral interventions in those who are obese.[139] Public health efforts seek to understand and correct the environmental factors responsible for the increasing prevalence of obesity in the population. Solutions look at changing the factors that cause excess food energy consumption and inhibit physical activity. Efforts include federally reimbursed meal programs in schools, limiting direct junk food marketing to children,[140] and decreasing access to sugar-sweetened beverages in schools.[141] When constructing urban environments, efforts have been made to increase access to parks and to develop pedestrian routes.[142]
Many countries and groups have published reports pertaining to obesity. In 1998, the first US Federal guidelines were published, titled "Clinical Guidelines on the Identification, Evaluation, and Treatment of Overweight and Obesity in Adults: The Evidence Report".[143] In 2006 the Canadian Obesity Network published the "Canadian Clinical Practice Guidelines (CPG) on the Management and Prevention of Obesity in Adults and Children". This is a comprehensive evidence-based guideline to address the management and prevention of overweight and obesity in adults and children.[68]
In 2004, the United Kingdom Royal College of Physicians, the Faculty of Public Health and the Royal College of Paediatrics and Child Health released the report "Storing up Problems", which highlighted the growing problem of obesity in the UK.[144] The same year, the House of Commons Health Select Committee published its "most comprehensive inquiry [...] ever undertaken" into the impact of obesity on health and society in the UK and possible approaches to the problem.[145] In 2006, the National Institute for Health and Clinical Excellence (NICE) issued a guideline on the diagnosis and management of obesity, as well as policy implications for non-healthcare organizations such as local councils.[146] A 2007 report produced by Sir Derek Wanless for the King's Fund warned that unless further action was taken, obesity had the capacity to cripple the National Health Service financially.[147]
Comprehensive approaches are being looked at to address the rising rates of obesity. The Obesity Policy Action (OPA) framework divides measure into 'upstream' policies, 'midstream' policies, 'downstream' policies. 'Upstream' policies look at changing society, 'midstream' policies try to alter individuals' behavior to prevent obesity, and 'downstream' policies try to treat currently afflicted people.[148]
Management
The main treatment for obesity consists of dieting and physical exercise.[68] Diet programs may produce weight loss over the short term,[149] but maintaining this weight loss is frequently difficult and often requires making exercise and a lower food energy diet a permanent part of a person's lifestyle.[150][151] All types of low-carbohydrate and low-fat diets appear equally beneficial.[152] The heart disease and diabetes risks associated with different diets also appear to be similar.[153] Success rates of long-term weight loss maintenance with lifestyle changes are low, ranging from 2–20%.[154] Dietary and lifestyle changes are effective in limiting excessive weight gain in pregnancy and improve outcomes for both the mother and the child.[155] Intensive behavioral counseling is recommended in those who are both obese and have other risk factors for heart disease.[156]
Three medications, orlistat (Xenical), lorcaserin (Belviq) and a combination of phentermine and topiramate (Qsymia) are currently available and have evidence for long term use.[157] Weight loss with orlistat is modest, an average of 2.9 kg (6.4 lb) at 1 to 4 years.[158] Its use is associated with high rates of gastrointestinal side effects[158] and concerns have been raised about negative effects on the kidneys.[159] The other two medications are available in the United States but not Europe.[160] Lorcaserin results in an average 3.1 kg weight loss (3% of body weight) greater than placebo over a year;[161] however, it may increase heart valve problems.[160] A combination of phentermine and topiramate is also somewhat effective;[162] however, it may be associated with heart problems.[160] There is no information on how these drugs affect longer-term complications of obesity such as cardiovascular disease or death.[157]
The most effective treatment for obesity is bariatric surgery.[163] Surgery for severe obesity is associated with long-term weight loss, improvement in obesity related conditions,[164] and decreased overall mortality. One study found a weight loss of between 14% and 25% (depending on the type of procedure performed) at 10 years, and a 29% reduction in all cause mortality when compared to standard weight loss measures.[165] Complications occur in about 17% of cases and reoperation is needed in 7% of cases.[164]Due to its cost and risks, researchers are searching for other effective yet less invasive treatments including devices that occupy space in the stomach.[166]
Epidemiology
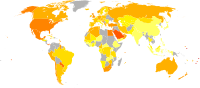
In earlier historical periods obesity was rare, and achievable only by a small elite, although already recognised as a problem for health. But as prosperity increased in the Early Modern period, it affected increasingly larger groups of the population.[168] In 1997 the WHO formally recognized obesity as a global epidemic.[81] As of 2008 the WHO estimates that at least 500 million adults (greater than 10%) are obese, with higher rates among women than men.[169] The rate of obesity also increases with age at least up to 50 or 60 years old[170] and severe obesity in the United States, Australia, and Canada is increasing faster than the overall rate of obesity.[19][171][172]
Once considered a problem only of high-income countries, obesity rates are rising worldwide and affecting both the developed and developing world.[32] These increases have been felt most dramatically in urban settings.[169] The only remaining region of the world where obesity is not common is sub-Saharan Africa.[2]



No comments:
Post a Comment